Structure, Function and Pain of the Knee
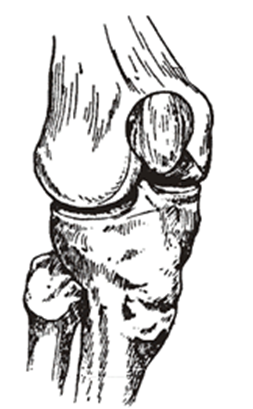
The knee can be described as a hinge joint and is the largest joint in the body. The knee joint is made up of:
- The kneecap (patella)
- Thigh bone (femur)
- Shin bone (tibia)
In a normal, healthy knee a smooth elastic tissue called articular cartilage lines and cushions the surfaces of the bones and allows them to move smoothly against each other. Lying between the femur and tibia are 'pads' of cartilage called menisci that act as shock absorbers to protect the bony surfaces. Ligaments like the anterior cruciate ligament (ACL) provide support for the knee in all directions and muscles like the quadriceps move the bones of the leg and provide strength.
The primary function of the knee is to transfer body weight down to the foot and to make walking more efficient by allowing the leg to bend and straighten. The ability of the knee to bend and straighten allows you to climb stairs, squat and bend to the floor and sit in a chair.
In an arthritic or damaged knee, often times the cartilage is destroyed and the smooth, bony surfaces become rough and irregular. These changes in the knee joint often cause pain, especially with walking and frequently result in a loss of movement of the knee. Swelling may occur at the knee, and you may find the muscles around the knee begin to weaken and the knee feels stiff when moving.
For more information about arthritis, please visit The Arthritis Society.
Knee Replacement
Knee replacement is often considered when the pain in the knee becomes so severe that it begins to interfere with your sleep and your ability to carry out activities such as walking, working or sports. The goals of surgery are:
- To end or reduce your pain.
- To improve your knee movement and overall function.
- To improve your quality of life.
Knee replacement involves removing the damaged bone from your knee joint and selecting and fitting your new joint according to your individual size. The damaged bone of the femur and tibia is cut away and replaced by metal components, one inserted on the end of the femur and the other on the top of the tibia. A plastic liner is inserted between the two metal components. The back of the patella is resurfaced and a plastic button is attached to complete the new knee joint.
Risks and Benefits of Knee Replacement
With your decision to proceed with knee replacement, you will discuss with your surgeon the risks and benefits of this surgery. Since 1994, more than 250,000 knee replacements have been performed in Canada and millions worldwide. They have proven to be extremely durable. Ninety to ninety-five percent success rates at ten- to twenty-year check-ups are common.
As with any operation, knee replacement has a number of potential risks. These include:
- Anesthetic complication
- Medical complication
- Deep vein thrombosis (DVT) and pulmonary embolism (PE) (blood clots in your leg or lung)
- Death (0.2%)
- Infection (approximately 0.5%)
- Slow healing
- Technical complication (i.e., damage to the skin, muscle, bone, nerve or blood vessel)
- Post-operative stiffness
- Post-operative pain
- Late wear or loosening of the implant needing to revision (between 0.5 and 1% per year)
- Limp
Your surgeon will review these with you before your surgery and answer any of your questions.
Revision Knee Replacement
In patients over the age of 60 years, it is hoped that a knee replacement will last the lifetime of a patient. Occasionally, the parts fail for a variety of reasons such as wearing out, loosening, instability or deep infection. A revision knee replacement often involves removing the parts put in previously and replacing this with new total knee parts.
Revision knee replacement is a more difficult and lengthy operation than the initial knee replacement but can offer extremely good results in terms of pain relief and return of function.
For more information regarding revision knee replacement, please consult with your orthopaedic surgeon.



