
Members of the surgical team are pictured with the new Hyperfine Swoop Brain Portable MRI system
March 9, 2026
A neurosurgery team at London Health Sciences Centre (LHSC), led by neurosurgeon Dr. Neil Duggal was the first in the world to use the Hyperfine Swoop Brain Portable MRI system during a surgery to remove a complex pituitary tumour this past October. During the patient’s surgery, an MRI was completed within the operating room to validate whether the tumor had been sufficiently removed, or if there was remaining residual mass that could be further removed before completing the procedure. The use of a portable MRI machine provided the neurosurgical team with immediate visibility within a highly complex area of the brain and afforded the patient greater confidence in the success of their surgical outcome.
The pituitary gland produces and releases hormones that control many bodily functions, including growth, metabolism, blood pressure, and reproduction. Most pituitary tumors are benign and slow growing, but because of their location and closeness to structures like the optic nerves, they can exert pressure and potentially affect brain function or vision as they grow.
For patient Dave Evans, who had been experiencing vision loss and headaches because of the tumour, learning the team had leveraged an MRI intraoperatively was reassuring news.
“When they explained to me that they used the MRI to confirm suspected residual mass, which then gave them the ability to clear out pretty much all of what could possibly be removed, I was very happy and relieved,” says Evans. “Hearing that it allowed them to move the dial from 90 to 99 per cent was incredible. It was the best, most timely care possible and gave me so much confidence in my recovery and longer-term outcome.”
For the surgical team it was another example of leveraging cutting-edge innovation as part of the Division of Neurosurgery’s commitment in providing the best possible care to the community.
“With the deep brain location of pituitary tumours, a surgeon is contending with complex anatomy during a resection,” says Dr. Duggal. “Around the tumour you have the carotid arteries on the left and right side and the optic nerves and chiasm sitting on the top. During minimally invasive, endoscopic surgery, it can be challenging to see the anatomical landmarks that help you confirm that you have removed as much tumor as is safely possible. Having access to a portable MRI during surgery was a game changer in our ability to be as precise as safely possible, within a single procedure.”
The images are read immediately in the operating room by the team to see if there is residual mass that could be safely removed, providing an important line of sight that isn’t possible during the procedure.
In addition to reducing the potential for patients to need a second surgery down the road, the portable MRI comes with other benefits including reducing the volume of imaging referrals for traditional MRI. It improves access by being able to be used in the intensive care unit, the neuro-observation unit and in our interventional neuroradiology suite.
Dr. Duggal adds, “Because the machine is portable and doesn’t have the same metal and safety considerations with its lower magnet strength, we can leverage it for multiple purposes across a range of our needs. In doing so, our team can potentially reduce some of the volumes we would have previously referred to our radiology department. It will not be appropriate for all neuro patient imaging needs, but by offsetting at least some of our imaging requests, we can help to potentially improve wait times for patients in other areas.”
Today, patient Dave Evans is doing well. His peripheral vision has been restored, and he no longer experiences the constant headaches.
Evans adds, “I’m grateful for the care I received at every turn. You could feel the kindness and commitment from everyone I met, from the person who cleaned my room, to the nurses, to the entire surgical team, and that was particularly helpful for me at a vulnerable time. I’ve received care in other hospitals, and my experience at London Health Science Centre was unrivalled. I know it played a role in helping to support my speedy recovery.”
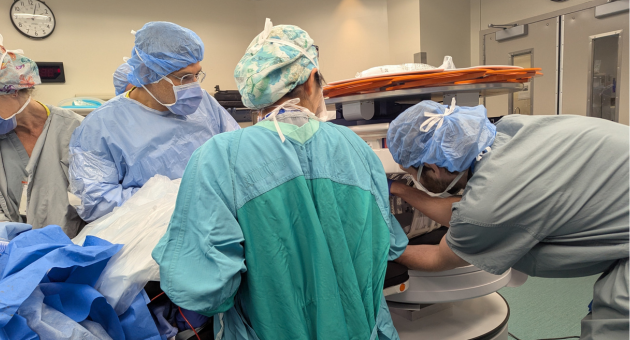
Members of the surgical team use the portable MRI in the operating room

Patient Dave Evans is pictured at LHSC in March 2026
Contact Information:
Jess Brady
Media Relations Consultant
London Health Sciences Centre
media@lhsc.on.ca
