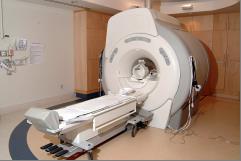
What is an MRI and why is my child having this done?
MRI stands for Magnetic Resonance Imaging and is a technique used to create an image of the inside of the human body. An MRI of the head shows how your child’s brain is made up in great detail and how it works. In people with epilepsy, the scan may help to find the cause of the seizures, such as a scar, lesion, or altered anatomy in the brain.
How does an MRI work?
The MRI machine uses a combination of magnetic fields and radio waves to create a very detailed picture of the brain. Due to the strong magnetic field, metal objects cannot be in or near the machine. For that reason, all metal objects such as earrings, will need to be removed. Your child will be provided with hospital pyjamas or a gown to ensure that no metal objects remain on their clothing. We do require ALL children to change into hospital clothing even if no obvious metal objects are seen, as we have had several instances of small metallic fibres woven into clothing. If your child has a surgical implant that contains metal, they may not be able to have an MRI scan. Please let our team know!
*Please Note: If your child has a vagal nerve stimulator (VNS), it is still safe to have an MRI. The Epilepsy Team needs to be notified as they will need to turn the VNS off during the scan. When the scan is complete, they will turn the VNS back on.
*Please remind your doctor if your child has braces. The scan may need to be delayed as braces can affect the quality of the image.
Sedated versus un-sedated MRI
An MRI of the head typically takes about 30 minutes and consists of a series of short scans with breaks in-between. During the scan, your child will need to lay on a platform that goes into a scanner. It is extremely important to lie still during the scan so that the machine can take the clearest and best pictures. If your child is able to lie still for the duration of the scan, they do not need a sedated MRI. Your child can choose a movie to watch during the scan and will be given a buzzer to hold so that they can let the technologist know how they are doing. The technologist will regularly check-in on them during the scan to ensure they are still comfortable and feeling well.
If your child is unable to lie still during the scan, they may need to have a sedated MRI. In that case, an appointment will be set up for a Pre-Admit Appointment in the Paediatric Medical Day Unit (PMDU). During this appointment, a paediatric anaesthesiologist (a doctor who will put your child to sleep) will have an in-depth conversation regarding your child’s medical history, family history with anaesthesia, a plan of care for the MRI, etc. Please come prepared to this appointment with any further questions regarding your child’s care under anesthesia.
*Note: If your child is having a sedated MRI they are not to have anything to eat or drink past midnight on the day of their scan. For the safety of your child, they must not have anything in their stomach before the doctor puts them to sleep.
On the day of the sedated MRI, your child will check in to the PMDU and have a quick height, weight, and vital signs (heart rate, blood pressure, oxygen saturation, respiration rate, and temperature) completed. The nurse will also go over any allergies, the last time your child ate/drank and your child’s overall well-being. If your child has a known respiratory illness such as the cold or flu, or has a fever, it may not be safe to continue with a sedated MRI that day. Once your child has changed into the hospital clothing, you will all be escorted down to the MRI suite where your child will be taken through the process of the MRI to help prepare them and can play in the Child life Room until it is their turn.
Do not worry – a nurse from the PMDU will call you with all of this information a few days prior to your appointment!
Once it is your child’s turn, one parent will be asked to accompany the child into the MRI suite. A Child Life Specialist may also be present to help distract and relax your child. Your child may sit in your lap or lay on the MRI platform while the anesthesiologist gives them a mask to breathe through. A sleeping medicine will be given through this mask and will help your child fall asleep initially. At this point, you can return to the waiting room until the scan is complete. While your child is asleep, the anaesthesiologist and his team will insert an IV (intravenous catheter) to administer the anaesthetic that will ensure your child remains asleep during the scan. An airway (oropharyngeal airway or laryngeal mask) will be inserted to maintain your child’s airway. Your child’s heart rate, blood pressure, oxygen saturation, and respiratory rate will be continuously monitored throughout. Since the MRI machine makes a loud knocking noise, earplugs will be placed in your child’s ears. Once the scan is complete, a specially trained paediatric post-anaesthesia nurse will take care of your child until they are awake. Once your child is awake, you will be called to the bedside for the remainder of the post-anaesthesia recovery. This process usually takes no more than half an hour. You will be discharged home straight from the MRI recovery room and the nurse will provide you with all the home care information prior to discharge.
What is the difference between an MRI and a CT scan?
A CT is a computerized axial tomography scan and uses x-rays to take pictures of the brain. A CT scan may be the only option if your child has a surgically implanted metal device. However, an MRI can typically produce a clearer and more detailed image than a CT scan.
What is a Functional MRI?
A functional MRI is used to see which parts of the brain are being used and how they are working while a patient is completing a language or movement task. In this case, the MRI machine is set up to look at how blood flows through the brain. The areas of the brain that are active during these tasks will have an increased blood flow and show up as bright colours on the scan.
In patients with epilepsy, a functional MRI may be used to see which parts of the brain are affected by seizure activity, what happens to their brain when a seizure occurs, and what role is played by structures near the part of the brain causing the seizures. It can also be used for patients who are considering an epilepsy surgery. Epilepsy surgery aims to remove the part of the brain that is causing the seizures to occur while minimizing removal of nearby structures. A functional MRI will see what that part of the brain does and what the effects of removing this area of the brain by surgery may have, improving safety and effectiveness of surgery.