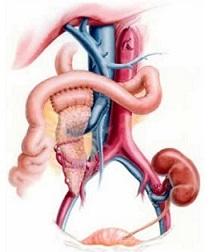
The pancreas is an elongated, irregularly shaped organ that is located behind the stomach.
The pancreas has two primary functions:
- exocrine function - produces enzymes, which are released into the intestine to digest food.
- endocrine function - produces insulin and glucagon, which are released into the bloodstream to help maintain normal blood sugar levels.
The specialized cells of the pancreas that produce insulin are called islet cells. Insulin lowers blood glucose levels in the body. When the islet cells stop producing insulin, the blood sugar rises uncontrollably and the patient develops diabetes.
Diabetes is the leading cause of end-stage kidney failure in North America. When blood glucose levels are constantly elevated, the kidneys' filtration mechanism becomes stressed. Their very small blood vessels become damaged, and the kidneys begin to leak. Without medical help, end-stage renal failure is life threatening.
Dialysis and insulin injections are treatments for patients with end-stage kidney disease and diabetes. These treatments, however, do not stop all the complications from diabetes, and kidney failure can become worse. If a kidney transplant alone is done, the majority of diabetic patients suffer through progression of diabetic eye, vascular, and nerve disease.
Kidney-pancreas transplantation is a surgical option for Type I diabetic patients with end-stage kidney failure. Pancreas-alone transplantation is performed to prevent the development of diabetic complications.
The Kidney-Pancreas Transplant Operation
Our transplant program provides three options for transplanting the pancreas, depending on the patient's needs.
The pancreas can be transplanted:
- simultaneously with a kidney from the same donor;
- after a living or deceased donor kidney transplant; or
- transplanted alone.
With simultaneous kidney-pancreas transplantation, the recipient undergoes one operation that uses both organs from the same donor. With pancreas after kidney transplantation, the recipient undergoes two separate operations from two different organ donors. Pancreas-alone transplants are performed to prevent the development of diabetic complications.
Kidney-pancreas transplant surgery takes between four and six hours. During this operation, the donor kidney is inserted and attached through an incision in either the right or left lower abdomen. The surgeon attaches the artery and vein of the new donor kidney to the iliac artery and vein, then attaches the ureter to the bladder. The recipient's own kidneys remain in place. The donor pancreas is placed in the abdomen and attached to either the bowel or bladder. Generally, the recipient’s own pancreas remains in place and is not removed because it continues to supply digestive enzymes and perform exocrine functions.
In the recovery room, the pulse, blood pressure and respiratory rate are monitored. Urine output is measured because that gives the staff an indication of how well the new kidney is functioning. They also monitor the blood sugar level, which indicates the immediate production of insulin by the transplanted pancreas. Most of the patients are transferred to the Multi-Organ Transplant Unit one or two hours after surgery.
Quality of Life
Successful kidney-pancreas or pancreas transplants dramatically improve the quality of patients' lives. A new pancreas provides regulated insulin production and cures the diabetes, and the new kidney eliminates the need for dialysis. Simultaneous kidney-pancreas transplantation has a one-year survival rate of 84% for the pancreas graft and 91% for the kidney graft. At three years, 80% of pancreas grafts are still functioning. Overall, a combined kidney and pancreas transplant will last an average of 12 to 15 years.


