|
SEDATIVES Sedatives are drugs that help to reduce anxiety. At higher doses, they promote sleepiness. They may also help people to forget uncomfortable experiences within the critical care environment. Patients may need sedatives to slow down a fast breathing rate or to make it easier to breath for the patient who is on a ventilator. The goal for sedation is to keep the patient calm and comfortable, while still remaining able to open their eyes and obey commands. We use a scoring tool to rate the patient's level of calmness and awareness. This is used to determine how much drug to give. We may need to heavily sedate patients during times of critical illness, as a way to rest their heart, lungs and brain, or to help the ventilator to work. Midazolam and lorazepam belong to a group of drugs called benzodiazipines They are similar to valium. These are the sedatives we use most frequently. These are usually given directly into the patient's bloodstream though an intravenous. Intravenous medications are used because they work immediately and eliminate the need to pick the patient with needles. Intravenous doses that are given intermittently are called "boluses". An intravenous bolus works immediately, and provides pain relief for a short period of time. If a patient has severe anxiety, or requires frequent bolus administration, sedatives may be given by continuous intravenous infusion by an infusion pump.
|
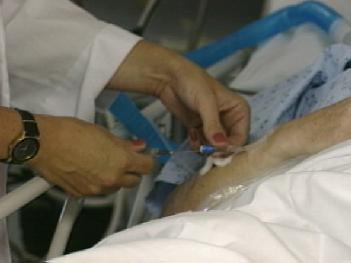
ABOVE: An intravenous bolus. |
|
|
|
|
|
|
|
|
|
|
|