|
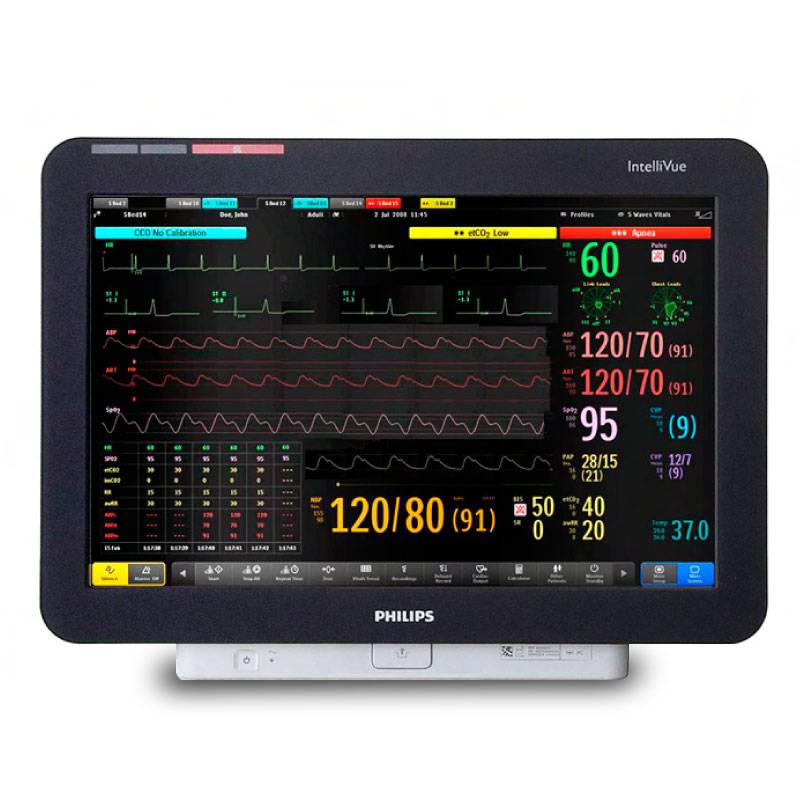
MONITORING The term monitoring means to "watch". Patients are admitted to a critical care unit because they require "intensive observation ". The nurse-patient ratio in a critical care unit is higher than in other areas of the hospital in order to meet the increased monitoring requirements of patients who are experiencing a serious health crisis. The critical care nurse is responsible for the ongoing monitoring of the patient on a 24 hour per day basis. Nurses monitor many aspects of the patient's condition. Although the increased technology in the critical care environment makes some of the monitoring requirements quite visible, technological monitoring is only one part aspect. Nurses continually observe and assess a patient's physical appearance and perform clinical assessments. They monitor the patient's physical and emotional response to treatment and identify patterns and trends. They adjust medications and treatments in order to achieve desired outcomes and watch for signs of patient discomfort and anxiety. Nursing care is individualized and adjusted according to the nurse's assessment findings. The goal is to achieve the best possible outcomes while minimizing the risk for complications. Patients who are critically ill often have problems that affect many body systems. Patients often have overlapping problems that complicate their treatment plans. Part of the complexity of monitoring in critical care is the need to integrate all of the information and interpret it within the context of the patient's unique situation. In addition to the ongoing monitoring that is performed by the nurse, patients are intermittently assessed by other members of the team. A respiratory therapist is assigned to each patient and will make regular rounds to assess the patient's breathing and adjust the ventilator. The CCTC pharmacist monitors the patient's medication profile and identifies ways to enhance the medication plan. The nutritional needs and orders are evaluated and adjusted by the dietitian, and patients are assessed and treated as required by the physiotherapist. The entire plan is monitored by one of the CCTC physicians. The patient's nurse is the central communication link in the patient's treatment plan. A patient's condition often changes frequently throughout the day. Observations are shared with other members of the team on an ongoing basis, in order to keep other health professional up-to-date regarding the patient's condition and plan of care. Critical care has a strong team of health professionals. Collectively the team brings many different perspectives and a broad base of expertise. The team meets daily to discuss observations and develop a comprehensive plan of care. VITAL SIGN MONITORING While the above data is generally collected as the minimum information, additional data is usually included when a critical care nurse collects "Vital Signs". For example, if the patient is on a ventilator or has continuous pressure monitoring, the Vital Sign check will include this information. Although "collecting Vital Signs" usually refers to the actual recording of data, vital signs are generally monitoring and displayed continuously in critical care. HEMODYNAMIC MONITORING
|
Last Reviewed: October 31, 2018