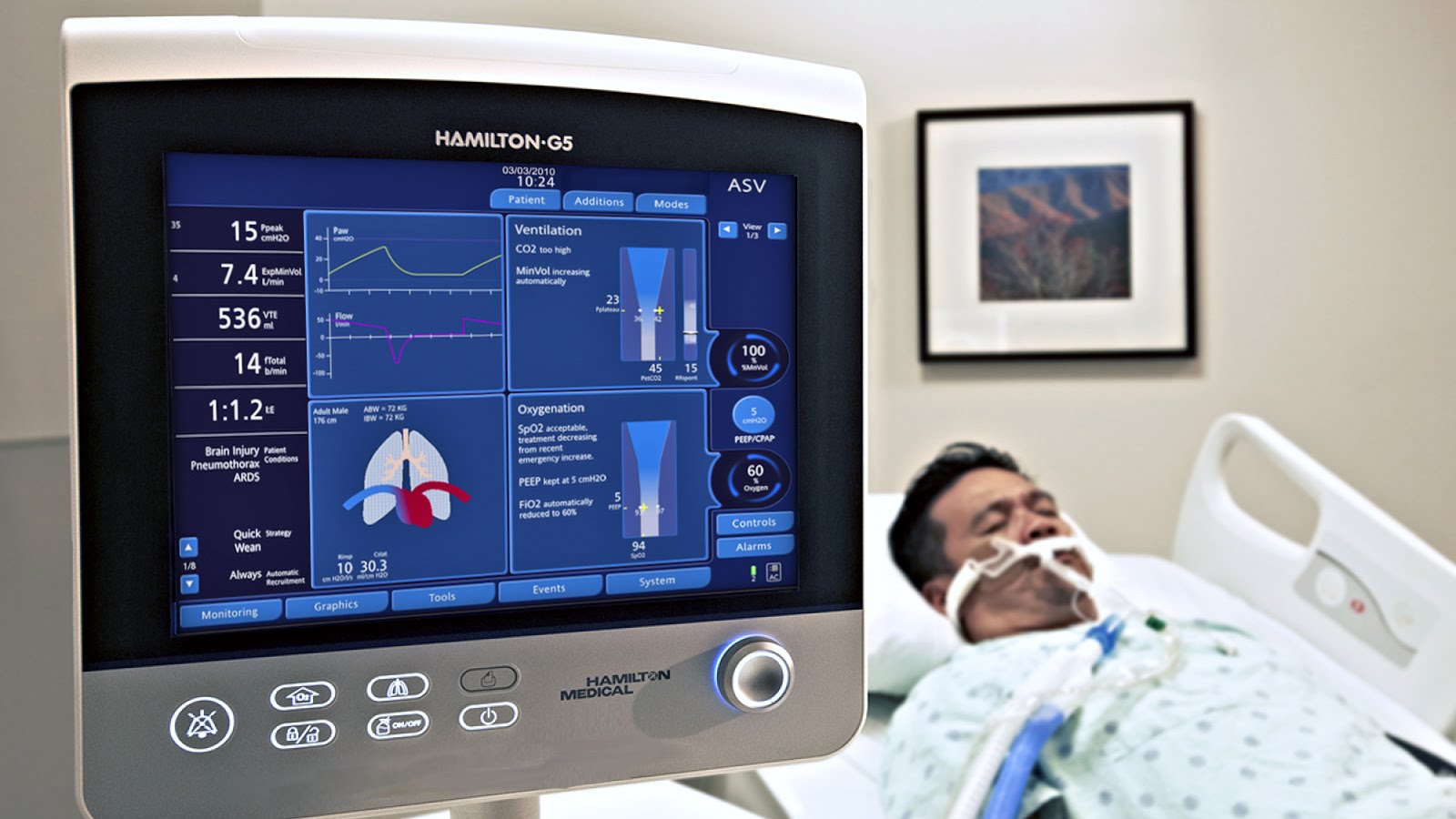
MECHANICAL VENTILATOR
The majority of patients admitted to critical care will need their breathing supported by a mechanical ventilator at some point in their admission. "To ventilate" means "to breathe". A mechanical ventilator is a machine that breathes for a patient. Although the term artificial "respirator" is sometimes used to describe a mechanical ventilator, this is really an incorrect term. The word respiration means "the exchange of gases".
A mechanical ventilator delivers breaths to patients, usually using positive pressure to assist or push a breath into the lungs.
We can fully ventilate a patient and make sure all of their breaths are delivered by the breathing machine (versus the patient). Continuous Mandatory Ventilation (CMV) is the most common method for fully ventilating a patient. In this type of breathing, the ventilator is set to give a minimum number of guaranteed breaths every minute.
SIMV (Synchronized Intermittent Mandatory Ventilation) is another way to breathe for a patient. With SIMV, the patient can breathe on their own in between a set number of guaranteed breaths. over and above the mechanical breaths. Patients can either be fully ventilated while on SIMV, or they can have a very low number of breaths. Setting the breath rate at a lower number forces the patient to breathe more on their own
Pressure Support (PSV or PS) is a common type of breathing support that is used when the patient needs partial support. We often use this when a patient begins to improve and we want to slowly reduce the amount of support from the ventilator. Our current ventilators provide Pressure Support in a mode called SPONT (for spontaneous). Spontaneous means the patient is initiating their own breathing.
With Pressure Support, the ventilator delivers an amount of positive pressure to the patient's airway as soon as the patient begins to breathe. This pressure makes it easier for the patient to take in a breath, and makes the breath larger.
The amount of Pressure Support delivered is measured in cmH20 and ranges between 5 (minimal support) and 30 (total support). Patients who only need 5 - 10 of Pressure Support may be ready to breathe without the ventilator. When patients need more than 15 of Pressure Support, they are not usually ready to come off the ventilator support completely. A pressure support over 20 is almost as much support as full mechanical ventilation.
Pressure Control is a way to give a mechanical breath to a patient while protecting the lungs from too high a pressure. Pressure Control is most frequently combined with CMV (P - CMV).
There are a variety of different ventilator settings than can be used to support a patient's breathing.
Oxygen (O2) is added to the air that is used to provide mechanical ventilation. Most patients need a higher concentration of oxygen than is present in normal atmospheric air.
When we breathe in, we bring fresh oxygen to our lungs. Normally, oxygen makes up 21% of all of the gases in the air that we breathe in. In normal health, this is enough incoming oxygen to keep the oxygen level in the blood at a level that meets the needs of all cells. The concentration of oxygen in the air that we breathe is called the FiO2 (Fraction of inspired oxygen). If a patient is not receiving any additional oxygen, we often say that the patient is on an FiO2 of .21 (21%) or "Room Air" (your and I are breathing room air unless we have supplemental oxygen).
A patient who is on more than 0.21 (21%) oxygen is receiving supplemental oxygen or Oxygen Therapy. Most patients in CCTC will need an FiO2 of .3 -.5. Patients who are very sick will need higher levels.
Oxygen is measured in the blood by a blood test called a "blood gas". The concentration of oxygen molecules in the blood is called the PaO2. We can also measure the amount of oxygen that is attached to the hemoglobin in red blood cells. This is called oxygen saturation (or SAT). If the amount of oxygen in the blood is lower than normal, the patient has hypoxemia (low oxygen in the blood).
Hemoglobin is a protein found inside red blood cells. We have about 300 hemoglobin molecules in every red blood cell. Each hemoglobin can attach a maximum of 4 oxygen molecules to its wall. If every hemoglobin molecule is carry the maximum number of oxygen molecules, the oxygen saturation reading is 100% (cannot be better than this). We usually try to keep oxygen saturation between 92-98%. We may keep it lower in some patients, for example those who have chronic lung diseases or patients who are requiring very high levels of oxygen.
We can intermittently measure oxygen saturation by doing a "blood gas" from a sample of arterial blood. This is a lab test that measures the oxygen, carbon dioxide, pH and bicarbonate levels in the blood. This is easiest to do when a patient has an indwelling catheter in an artery (called an arterial line). Arterial lines also provide continuous blood pressure measurement.
We continuously measure oxygen saturation in most patients in CCTC. This is done by taping or clippling an oxygen saturation probe onto a patient's finger or forehead. The oxygen saturation probe (SAT probe) reflects an infrared light beam into the blood vessels. The light that bounces off of the red blood cells will have different wavelengths based on the amount of oxygen attached. This information is used to display a continuous oxygen saturation reading (SPO2).
If a patients oxygen level remains low despite higher concentrations of inspired oxygen, we may need to increase the amount of pressure in the lungs in order to keep the small air sacs open. This type of pressure is maintained at the end of exhalation and is called Positive End Expiratory Pressure (PEEP).
Minute Volume, also called Minute Ventilation, is the total amount of air that is moved in and out of the lungs per minute. It is measured by the ventilator. Carbon dioxide is cleared during exhalation (when the minute volume is produced). If the amount of carbon dioxide in the patient's blood increases, we need to adjust the ventilator to move more air in and out per minute (increase the minute volume). The simplest way to do this for a patient who is receiving breaths from the ventilator is to increase the breathing rate (the AC or SIMV).
Carbon dioxide is one of the waste products that all cells of the body produce during metabolism. It is a weak acid. Carbon dioxide enters the blood stream from metabolizing cells and is carried to the lungs. When we exhale, carbon dioxide is removed from the body. If we are not breathing enough to meet our needs, the carbon dioxide level in the blood stream will increase. We adjust the amount of mechanical ventilation that we provide so that the patient's carbon dioxide and pH levels (measurements of acidity) are close to normal.
There is very little carbon dioxide in the air that we breathe in. If we measure the carbon dioxide level at the entrance of a breathing tube, the concentration will rapidly fall as we take in a breath.
During exhalation, the level of carbon dioxide rises as we blow it out of our body. We often measure the amount of carbon dioxide in the air that the patient exhales. We measure it at the very end of the breath as a way to monitor the effectiveness of mechanical ventilation. This is called the End Tidal CO2.
Tidal Volume is the size of a patient's exhaled breath. It is measured in cc's of air.
Last Reviewed: October 31, 2018