|
CARDIAC ARREST; The word cardiac means "heart" and "arrest" means stop. If the heart stops pumping for any period of time, the event is called a "Cardiac Arrest". If the heart stops pumping for > 5 minutes, the risk of brain damage increases. Resuscitation is a term used to describe efforts to restart the heart and restore normal circulation. Cardiac arrests are often referred to as "witnessed" or "unwitnessed" events . A cardiac arrest is called unwitnessed if the patient is found without a pulse and no one was present at the time the patient collapsed. Most cardiac arrests in a critical care unit will be "witnessed" because the patient is usually connected to a heart monitor (or ECG). Unwitnessed cardiac arrests carry a high risk for brain damage because patients have often gone longer than 5 minutes before resuscitation efforts were started. When a patient's heart stops beating, the first intervention is CardioPulmonary Resuscitation (or "CPR"). The first person to identify the cardiac arrest begins pressing on the patients chest in an effort to "squeeze" the heart and cause blood to flow. This is called "Chest Compressions" (Image 3). The patient is quickly connected to a heart monitor to find out the patient's electrical pattern. The pattern will help the team to decide the next steps to take. Ventricular Tachycardia (also called "VT" or V-Tach) is a type of electrical disturbance where the ventricles (or bottom chambers) being to beat very fast. If they beat too quickly (usually at rates > 200 beats per minute), the heart may become too ineffective to produce a detectable pulse. This type of rhythm can deteriorate quickly into a very chaotic quivering of the ventricles called Ventricular Fibrillation (also called VF or V-Fib) . During Ventricular Fibrillation, the heart is not pumping any blood at all. Ventricular Fibrillation is treated by a quick electrical shock that causes the heart to completely stop. The shock is usually delivered through paddles that are placed on the patient's chest. This procedure is called Defibrillation. Sometimes, if the heart is stopped completely, the heart will restart itself within a few seconds and return to a normal electrical pattern. Abnormal heart patterns that cause the heart to fire extremely fast usually originate from cells that are outside the normal electrical pathway. Sometimes, we may need to shock a heart to get it out of a very fast rhythm. If the patient has a pulse or blood pressure when we deliver the shock, the shock we deliver is called "cardioversion" . The main difference between defibrillation and cardioversion is "when" the shock is delivered. Defibrillation is used when the patient has no pattern to their electrical activity, therefore, the shock is delivered at any point in the rhythm. When cardioversion is used, the machine looks at the pattern, and delivers the shock between beats. Because the heart has usually been deprived of oxygen for a shorter period of time when cardioversion is used, the heart will often respond to a lower amount of electrical current. Cardioversion may also be performed in "non emergency" situations (called electively). If the situation is not urgent, the physician may discuss the planned cardioversion in advance. Because defibrillation is always a medical emergency, there is usually no time to explain the procedure before the patient is defibrillated. Cardioversion and defibrillation are performed using the same machine, and are done for the same purpose (to stop the heart and allow abnormal rhythm to return). Because of this similarity, health care professionals often used the two terms interchangeably. In addition to electrical shock, resuscitation efforts following cardiac arrest will usually include the administration of drugs to correct low blood pressure and may include medications to prevent abnormal rhythms from occurring. The patient may require extra fluid and may be placed on a mechanical ventilator. Occasionally, the patient may require an artificial pacemaker. |
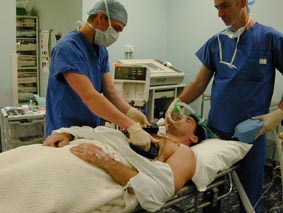
Image 1: |
|
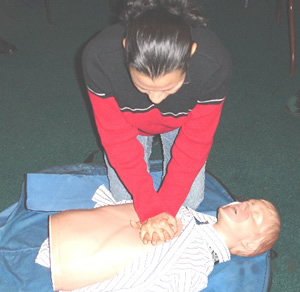
Image 2: |
|
|
Any patient who experiences a cardiac arrest may suffer some brain damage. The risk for damage increases the longer It takes to restore the patient's circulation. The likelihood of restoring the circulation is better if the patient has a short period of cardiac arrest or has Ventricular Tachycardia or Ventricular Fibrillation that responds to the initial electrical shock. Successful resuscitation is less likely in patients who fail to respond to treatments quickly or who have no electrical rhythm (called "asystole" for "no beat"). Patients who are very elderly, have previous brain damage or have many other medical problems are less likely to have a good quality of survival. Because a cardiac arrest carries the risk of brain damage, there may be times when the doctor will ask you to consider whether we should initiate aggressive treatments in the event of a cardiac arrest. You may also wish to initiate this discussion if you do not believe the patient would want this type of treatment performed. Do not hesitate to discuss the situation with the doctors and nurses. The decision to withhold certain medical procedures is a very difficult one to make on behalf of another person. Your should never feel rushed or pressured. Talk about the situation with the other members of your family and with the nurses and doctors. You may find it helpful to talk with the unit social worker. Try to imagine what your family member would say if they had the same information presented. Decisions to withhold certain medical procedures do not need to be thought of as "all or none". You may decide that you do not want compressions performed, however, you want everything else continued up to that point. Decisions need to be made that are individualized to your family members medical condition and to your family's wishes. Talk to the nurses and doctors to explore different options.
|
|
|
Image 3: |
|
|
|
Last Reviewed: October 23, 2014